Resuscitation
Transcranial ultrasound has been studied in the acute (even prehospital!) management of trauma including TBI, cardiac arrest, post-ROSC patients, cardiogenic shock, septic shock, hypovolemic shock, hepatic encephalopathy, stroke, intracranial hemorrhage, and the list goes on.
If you only had time to understand one extra concept in order to gain the best understanding of the research and be able to apply it--or decide not to--that concept would be the Pulsatility Index. Specifically, the Gosling Pulsatility Index. Skip this next section if you already have a handle on it.
The Gosling Pulsatility Index
Don't panic! The machine may calculate this on its own. If not, I'll show you how to force it to.
So what does the Ryan Gosling Pulsatility Index tell us?
It gives us a number that reflects distal cerebrovacular resistance and compliance.
How to Get One
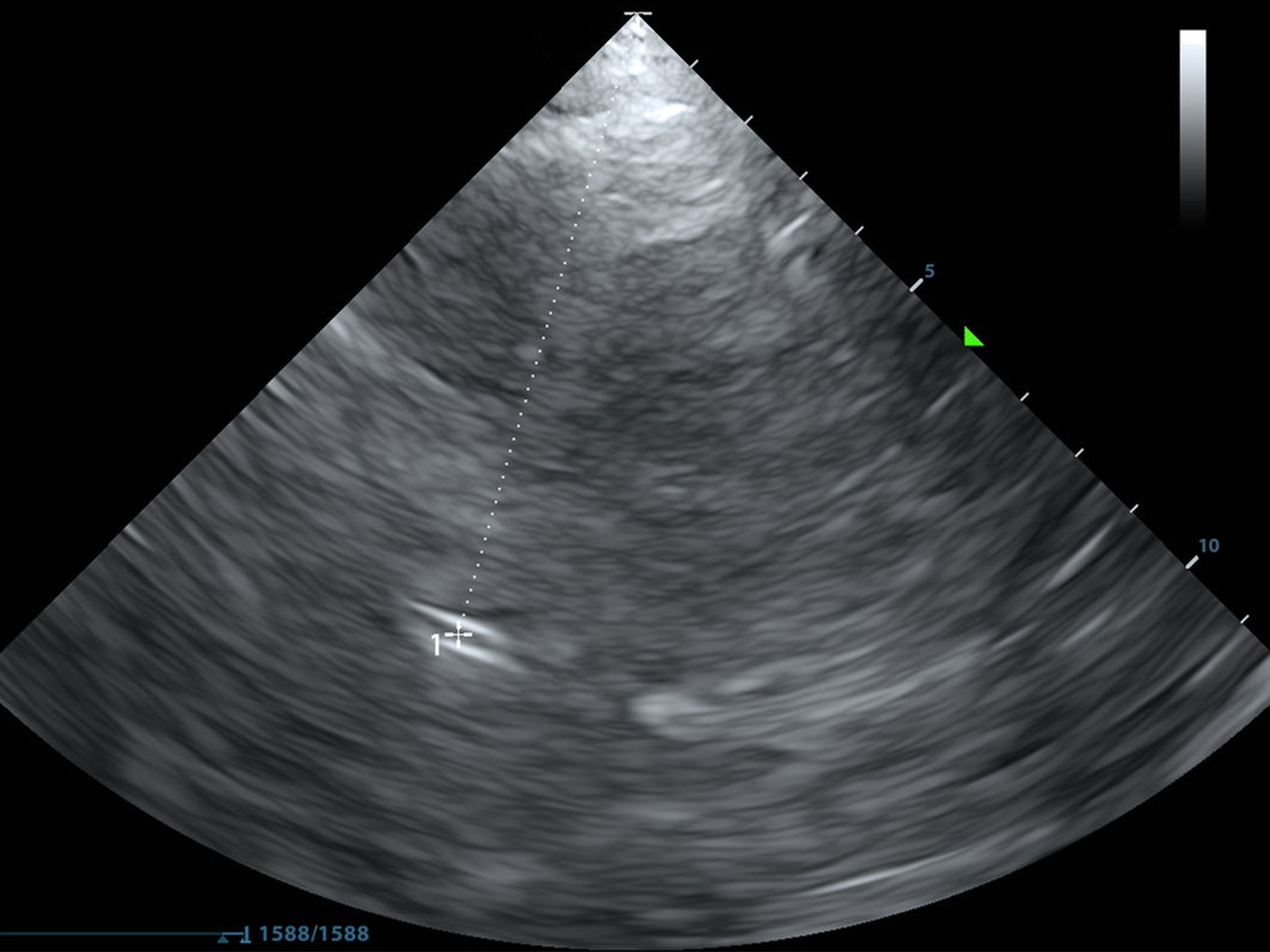
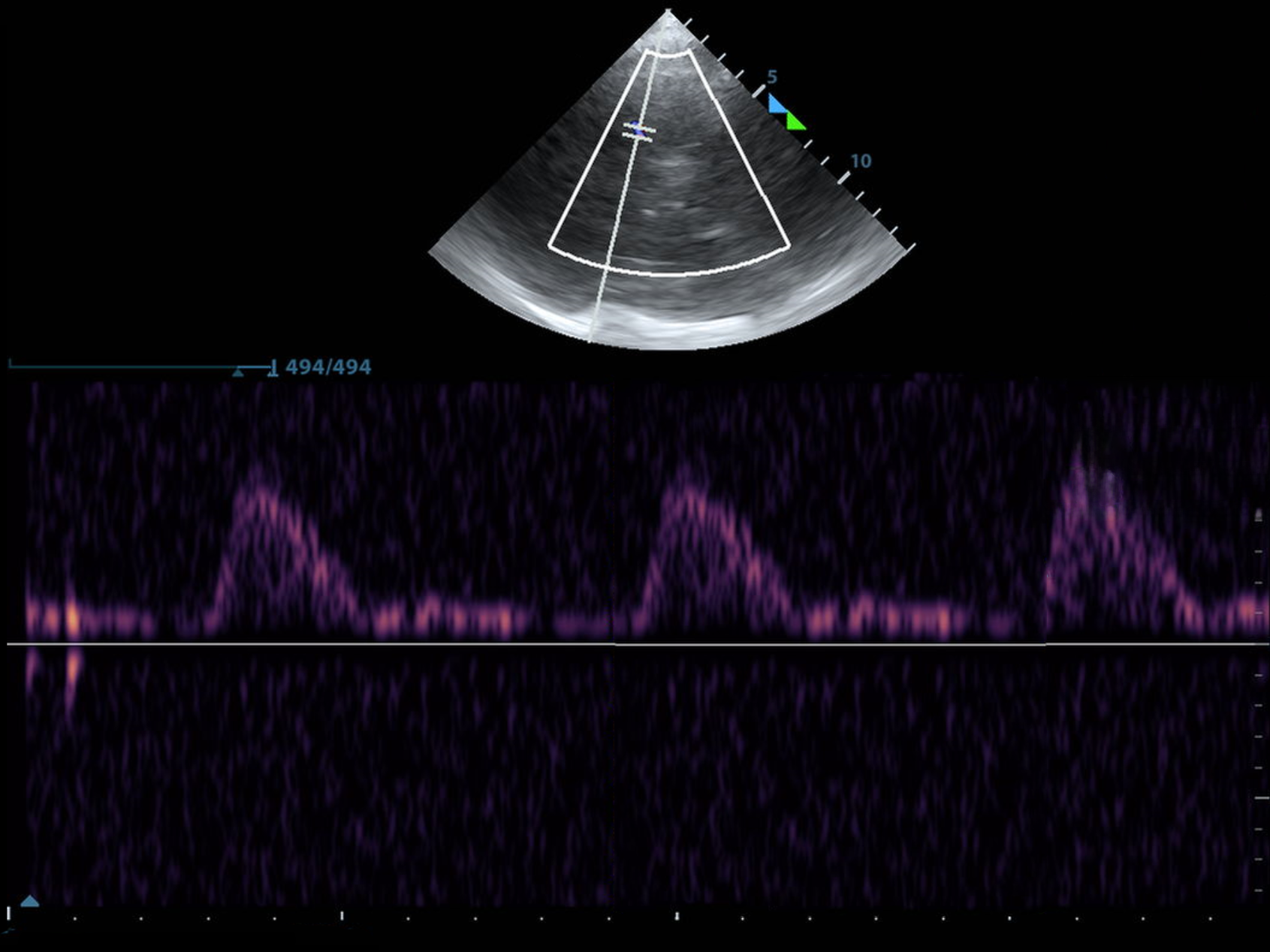
Below, you'll find a normal MCA PI. It's also majestic, virile, ruggedly-handsome, and mine.
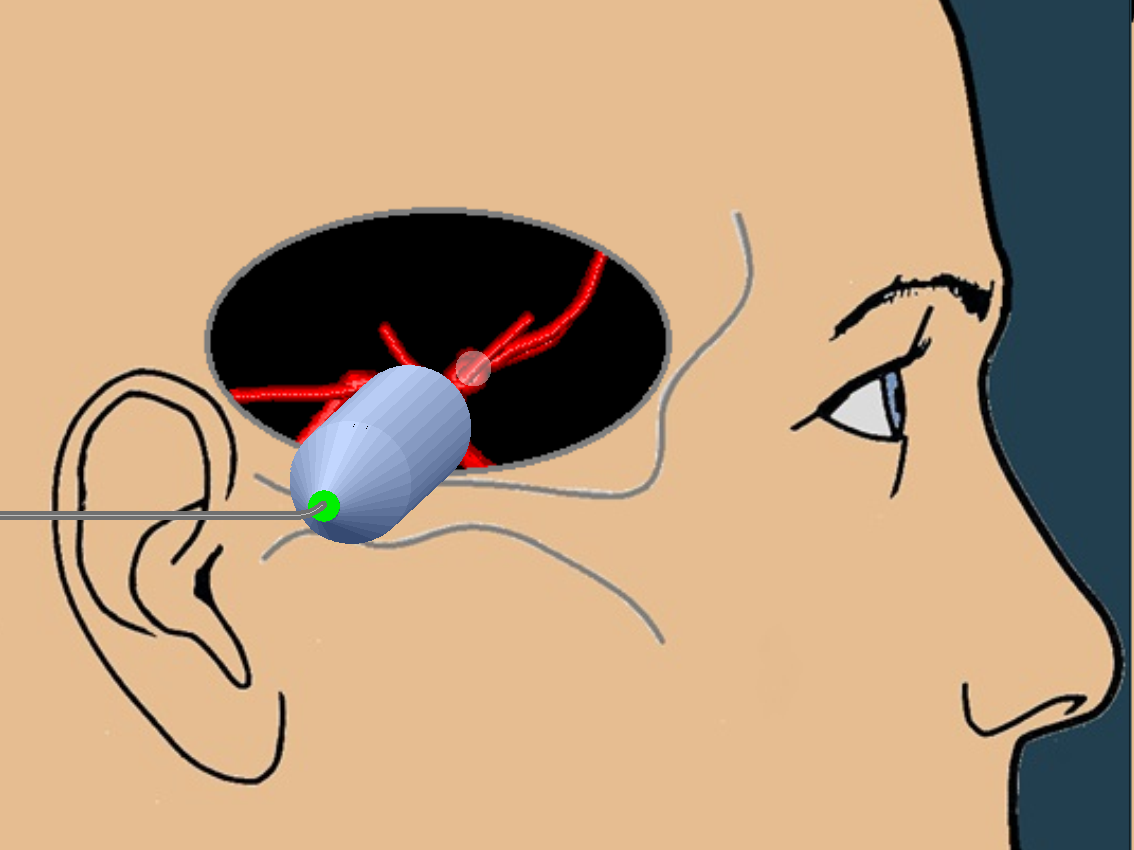
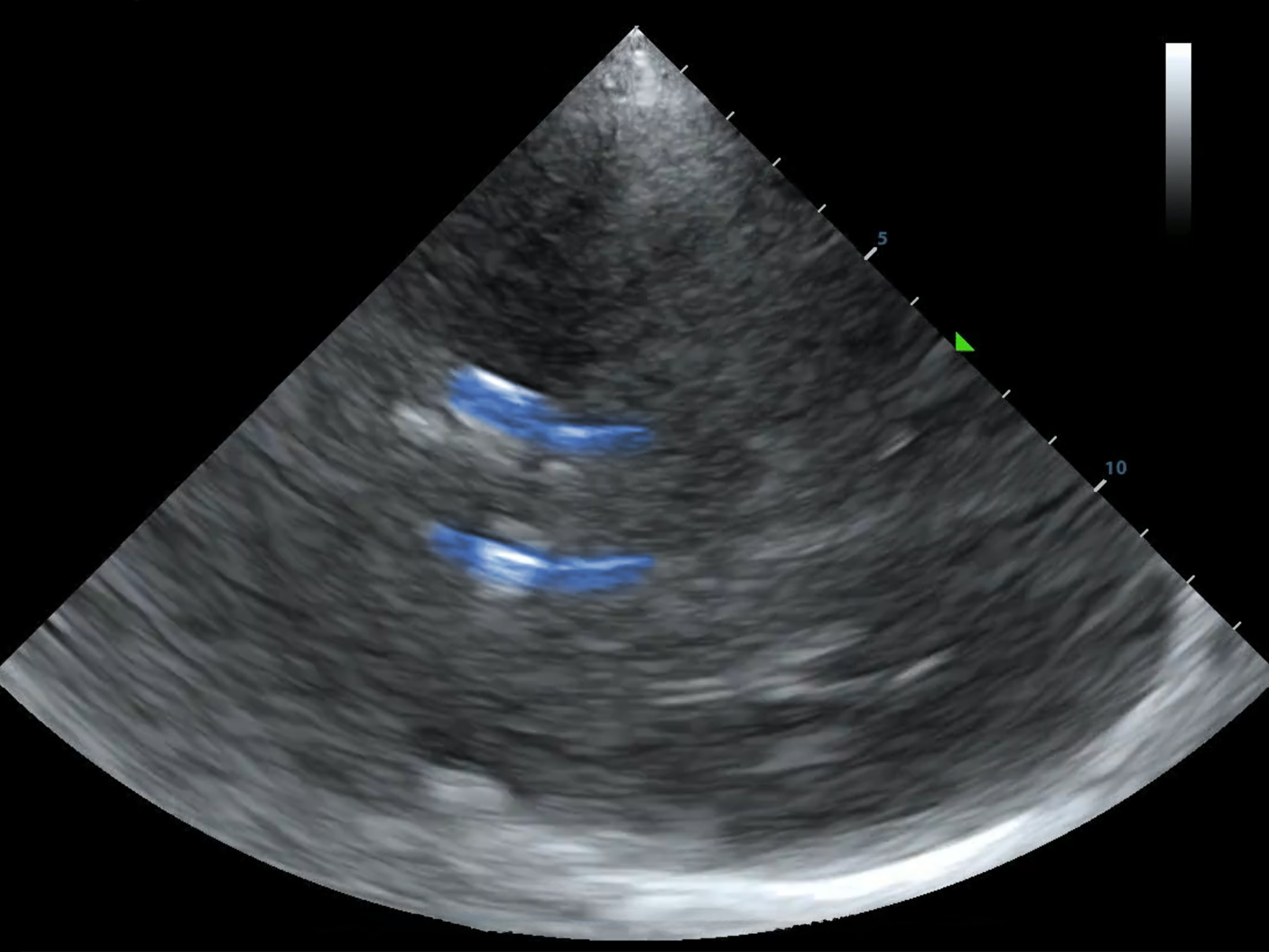
As always, I found the MCA with color doppler and put the pulse wave doppler gate on the proximal MCA.
I selected "AutoTrace" and dragged the line from the beginning of the systolic upstroke until end diastole and the machine calculated the rest.
You can also trace the waveform with a cursor, or some machines trace it and provide the calculations without you even asking!
TCD-Guided Resuscitation:
Sepsis
What We Know So Far
ICU-based studies suggest that cerebrovascular autoregulation is impaired in 66-83% of severe sepsis, septic shock, and sepsis-associated encephalopathy (SAE) patients who warranted ICU level of care[1,2].
This impairment is worse earlier in the patient's clinical course and has a high association with poor neurological outcomes including permanent disability[3].
Fluid resuscitation in septic patients improves systolic blood flowing in the middle cerebral artery, but does not improve diastolic blood flow--which is crucial to adequate perfusion of the brain[4].
In a new RCT, titration of norepinephrine to a goal of PI <1.3 in these patients resulted in significantly fewer episodes of cerebral hypoperfusion, higher MAPs once off of pressors, and higher GCS upon leaving the ICU compared to a control group with traditional MAP >= 65 goals[5].
Álvarez-Fernández, J. A., & Pérez-Quintero, R. (2009). Use of transcranial Doppler ultrasound in the management of post-cardiac arrest syndrome. Resuscitation, 80(11), 1321–1322. https://doi.org/10.1016/j.resuscitation.2009.07.011
What it Could Mean
Studies into sepsis and cerebral perfusion do not extrapolate directly to the point-of-care or the ED. We just aren't scanning the brain yet. However, these cerebral autoregulation and perfusion problems are worse earlier in the clinical course--and they're likely present when we meet our patient, even if we aren't looking.
Pressor titration goals of PI <1.3 and MAP >= 65 are not mutually exclusive.
Sepsis patients pressor-elevated MAPs as high as 98 did not demonstrate evidence of abnormally high intracranial arterial velocities or blood flow [7]. While this is not safety data, there is evidence that a MAP of 70 may not cause the patient to disintegrate.
Surviving Sepsis gave us guidelines from robust systemic hemodynamic data. It did not tell us whether our resuscitation was sufficient according to the brain.
While there is insufficient research to integrate PI <1.3 goals into clinical practice in the ED, or perhaps even the ICU, it also appears that one could do so while still practicing according to the Standard of Care. If a MAP of 75 gets the patient a PI just under 1.3, for example, then maybe "above 65" is good enough and we leave the pressors alone for a little while.
1. Schramm, P., Klein, K. U., Falkenberg, L., Berres, M., Closhen, D., Werhahn, K. J., David, M., Werner, C., & Engelhard, K. (2012). Impaired cerebrovascular autoregulation in patients with severe sepsis and sepsis-associated delirium. Critical Care, 16(5), R181. https://doi.org/10.1186/cc11665
2. Taccone, F. S., Castanares-Zapatero, D., Peres-Bota, D., Vincent, J.-L., Berre’, J., & Melot, C. (2010). Cerebral Autoregulation is Influenced by Carbon Dioxide Levels in Patients with Septic Shock. Neurocritical Care, 12(1), 35–42. https://doi.org/10.1007/s12028-009-9289-6
3. Cucciolini, G., Corda, I., Forfori, F., & Corradi, F. (2024). Brain Ultrasonography in Critically Ill Septic Patients: A Scoping Review. Journal of Clinical Medicine, 13(22), 6920. https://doi.org/10.3390/jcm13226920
4. de Goede, A. A., Loef, B. G., Reidinga, A. C., & Schaafsma, A. (2017). Fluid Resuscitation in Septic Patients Improves Systolic but not Diastolic Middle Cerebral Artery Flow Velocity. Ultrasound in Medicine & Biology, 43(11), 2591–2600. https://doi.org/10.1016/J.ULTRASMEDBIO.2017.06.027
5. Salem, M. S., Abosabaa, M. A., Abd El Ghafar, M. S., EI-Gendy, H. M. E.-D. M., & Alsherif, S. E. I. (2025). Norepinephrine titration in patients with sepsis-induced encephalopathy: cerebral pulsatility index compared to mean arterial pressure guided protocol: randomized controlled trial. BMC Anesthesiology, 25(1), 5. https://doi.org/10.1186/s12871-024-02814-0
6. Matta, B. F., & Stow, P. J. (1996). Sepsis-induced vasoparalysis does not involve the cerebral vasculature: indirect evidence from autoregulation and carbon dioxide reactivity studies. British Journal of Anaesthesia, 76(6), 790–794. https://doi.org/10.1093/bja/76.6.790
7. Matta, B. F., & Stow, P. J. (1996). Sepsis-induced vasoparalysis does not involve the cerebral vasculature: indirect evidence from autoregulation and carbon dioxide reactivity studies. British Journal of Anaesthesia, 76(6), 790–794. https://doi.org/10.1093/bja/76.6.790
TCD-Guided Resuscitation:
TBI
What We Know So Far
The proposed Ultrasound-Guided Cardio-cerebral Resuscitation (UGCeR) protocol offers a methodical approach to managing inadequate cerebral blood flow detected in patients with severe TBI suggestive of increased intracranial pressure and poor perfusion--even in patients without midline shift or intracranial hemorrhage [1].
Tamagnone, F. M., Cheong, I., Luna, E., Previgliano, I., & Otero Castro, V. (2023). Ultrasound-guided cerebral resuscitation in patients with severe traumatic brain Injury. Journal of Clinical Monitoring and Computing, 37(2), 359–363. https://doi.org/10.1007/s10877-022-00954-7
1. Tamagnone, F. M., Cheong, I., Luna, E., Previgliano, I., & Otero Castro, V. (2023). Ultrasound-guided cerebral resuscitation in patients with severe traumatic brain Injury. Journal of Clinical Monitoring and Computing, 37(2), 359–363. https://doi.org/10.1007/s10877-022-00954-7