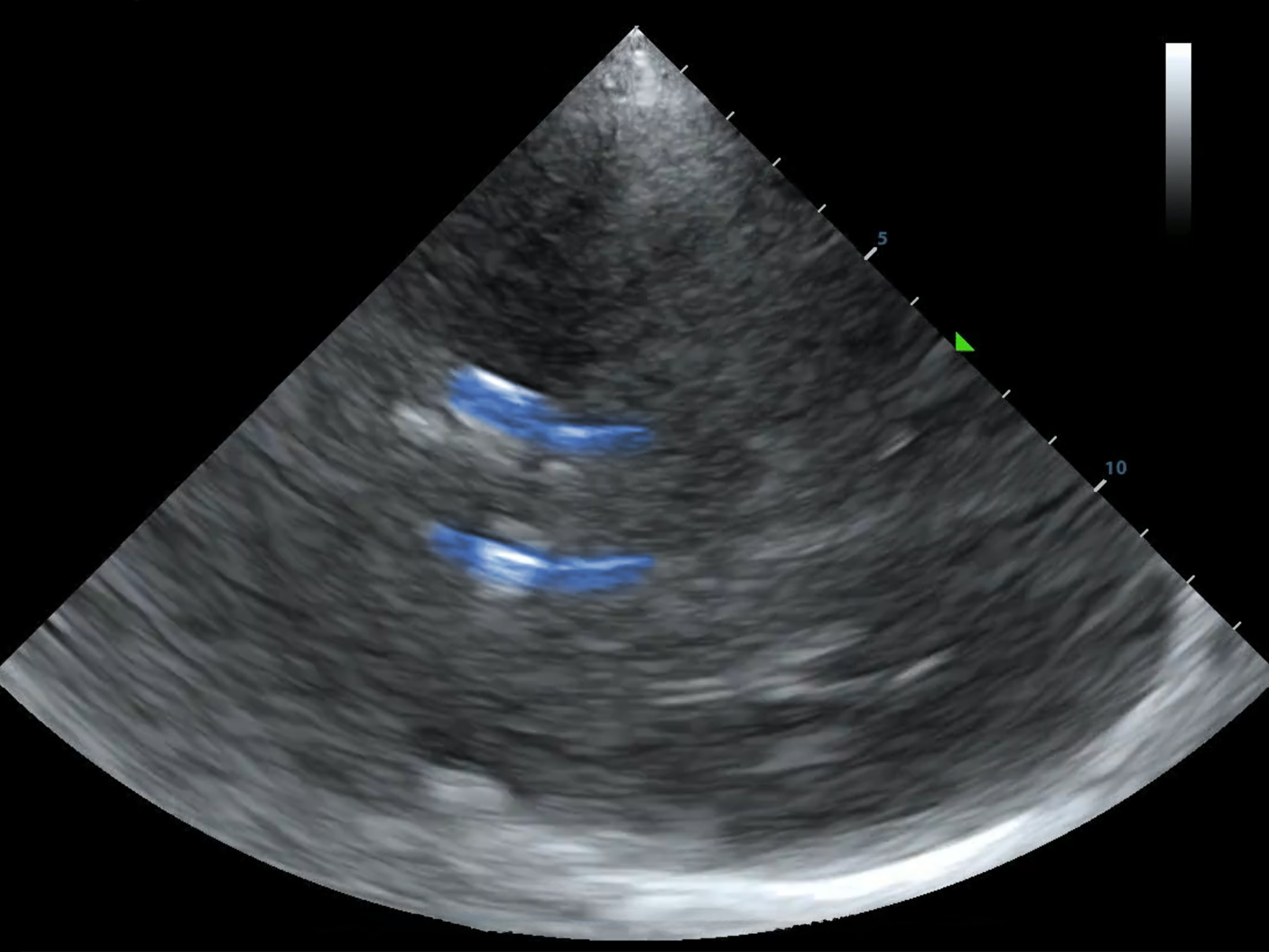
The ability to rapidly assess cerebral circulation and brain function using transcranial ultrasound (TCD/TCCS) is an exciting advancement that can transform bedside assessment in the prehospital setting, in the ER, and on the wards. It is not new, the data is often robust, and you can do it with the ultrasound you already have. Here’s why you should be interested:
1. Rapid, Non-Invasive Neurological Assessment
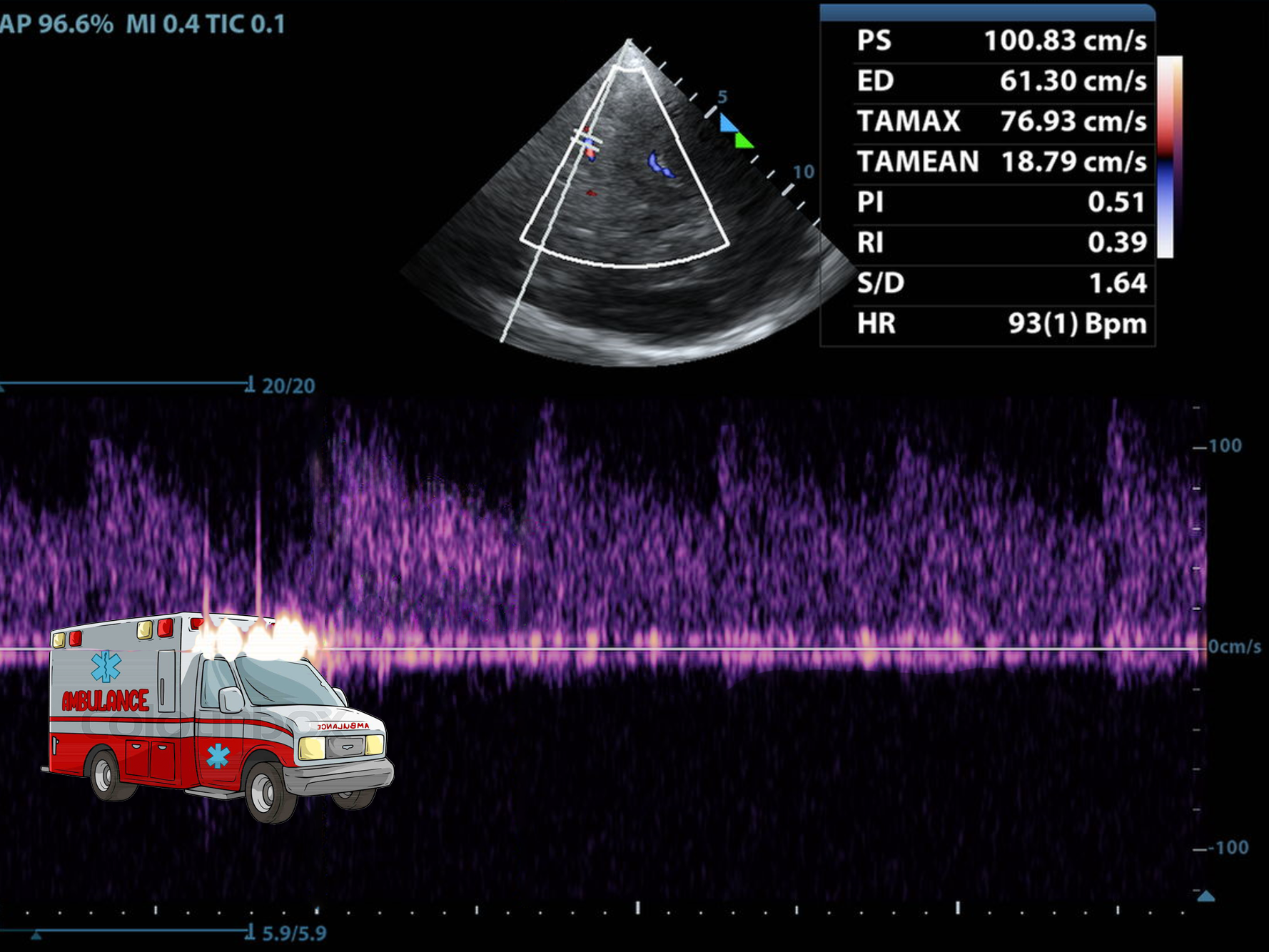
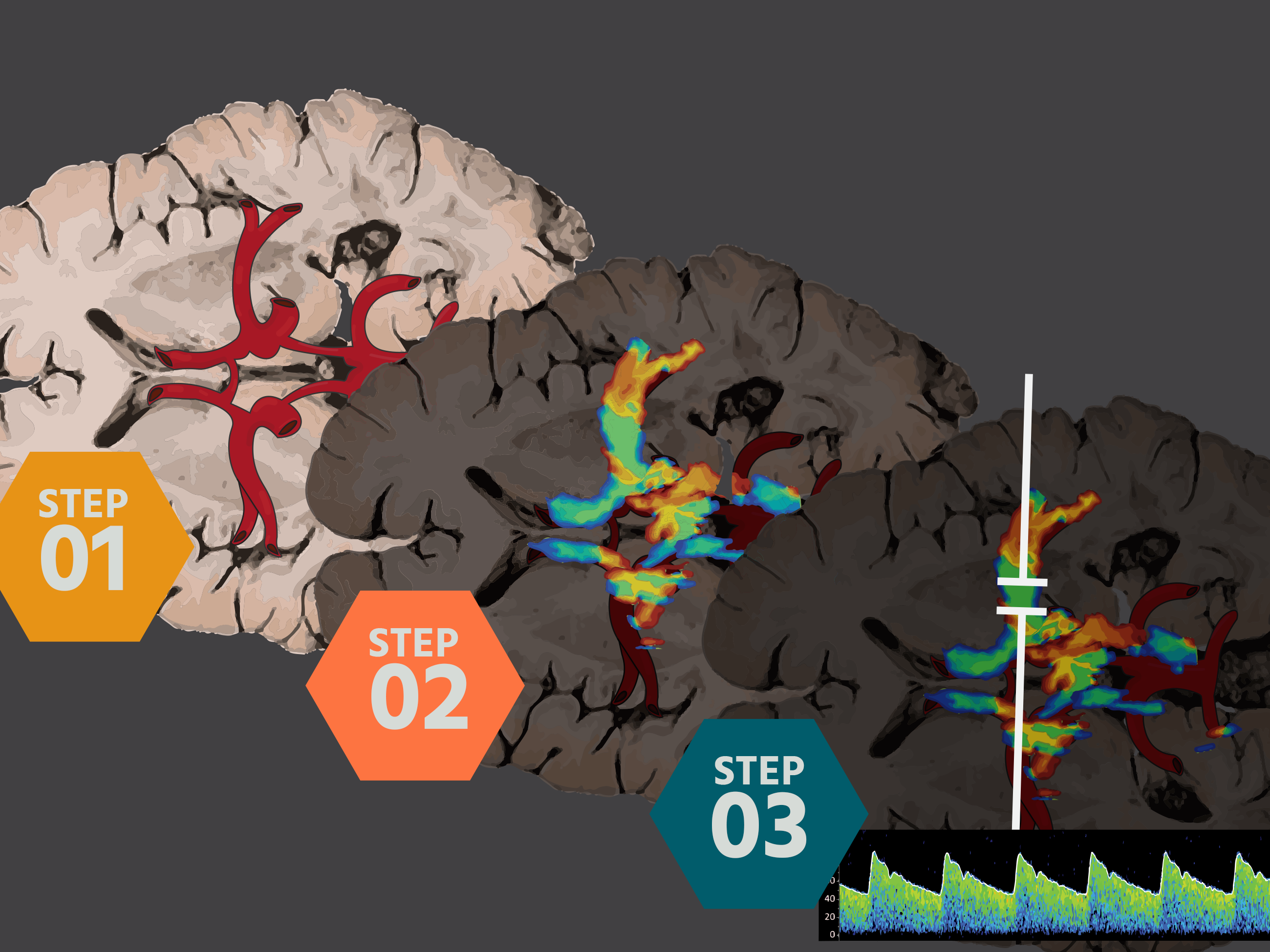
Transcranial ultrasound provides real-time information about cerebral blood flow and perfusion, allowing us to evaluate stroke, traumatic brain injury, increased intracranial pressure, and vasospasm in a matter of minutes and make timely decisions about hyperosmolar therapy. Though it does not replace CT or MRI, these modalities require patient transport and involve delays--bedside ultrasound fits into the spaces between 3D imagine.
2. Early Detection of Increased Intracranial Pressure (ICP) and Midline Shift
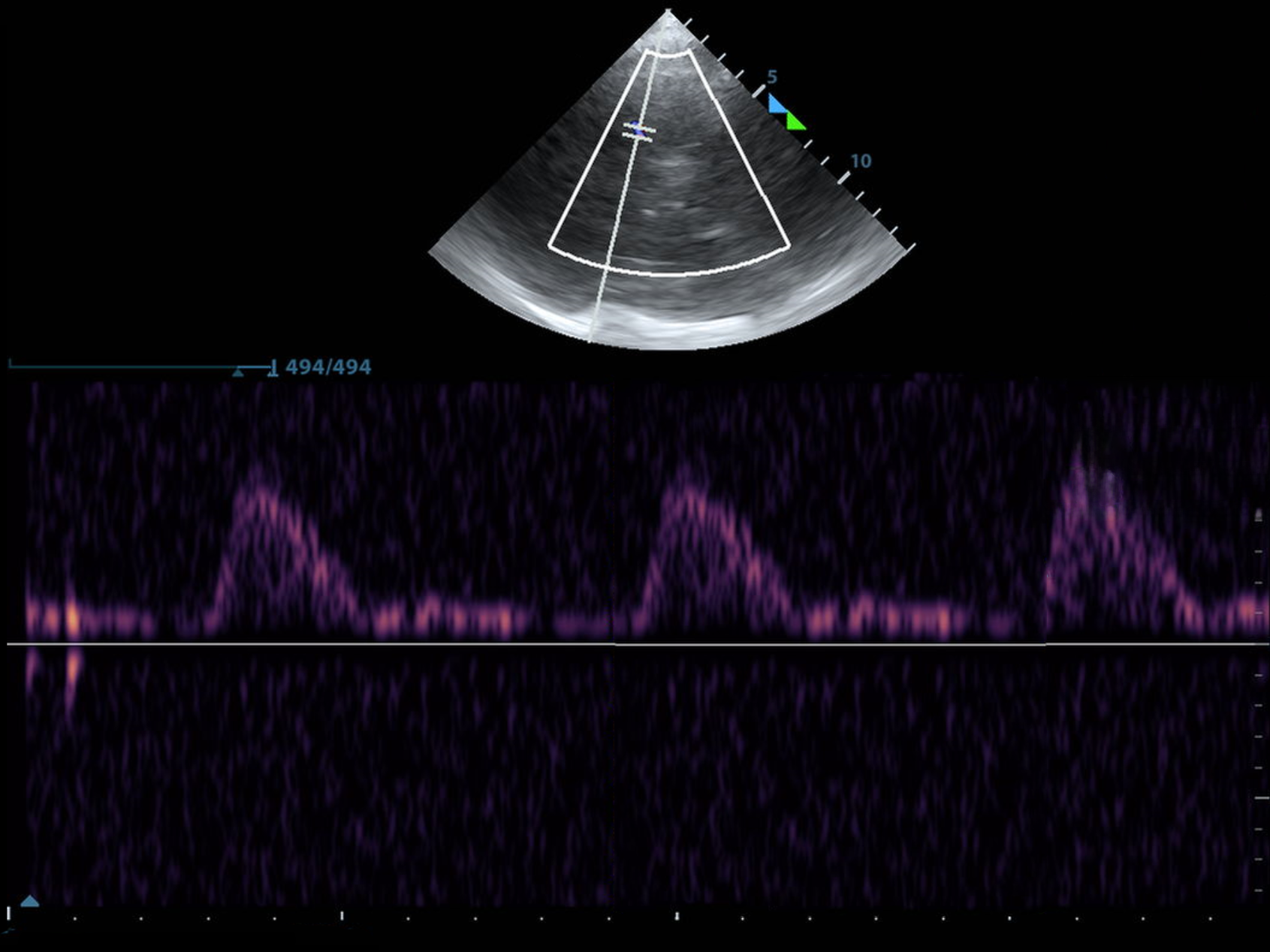
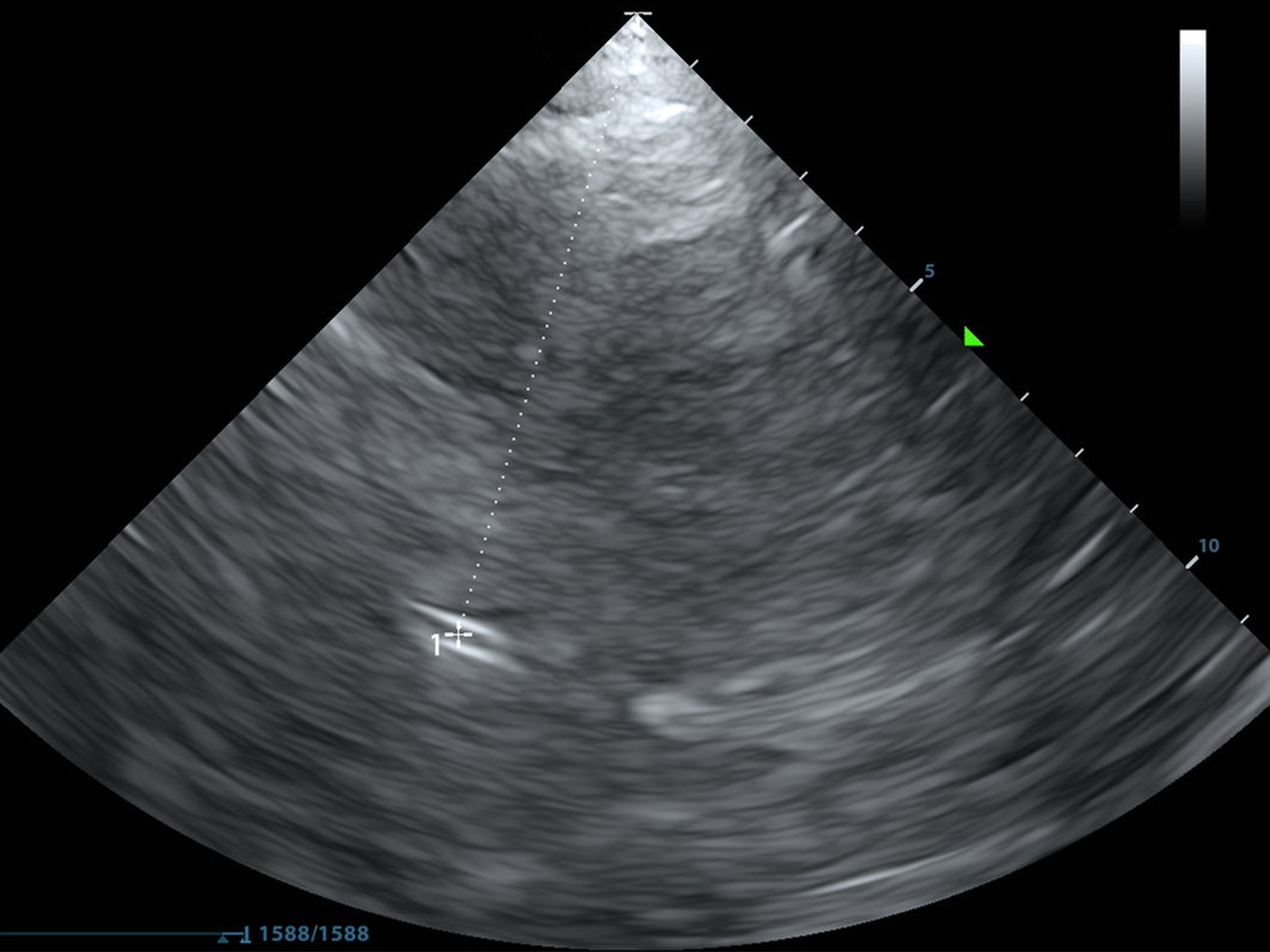
Many neurological emergencies involve increased ICP, from trauma to hemorrhage. TCD can detect signs of rising ICP and impending herniation through waveform analysis, and can detect midline shift with greyscale images alone, allowing us to make timely decisions about interventions such as hyperosmolar therapy or neurosurgical consultation. It is fast and it is repeatable.
3. "Whole Body" POCUS
We are already familiar with point-of-care ultrasound (POCUS) for FAST exams, cardiac evaluation, and vascular access. Learning transcranial ultrasound is a natural extension, providing us a Brain Echo to assess cerebrovascular status alongside systemic resuscitation efforts.
4. The Brain is the Big Bottleneck in Cardiac Arrest Care
Multiple studies, such as PARAMEDIC 2, have shown us that, in cardiac arrest, we are able to save a patient's heart far more often than their brain. Transcranial ultrasound can give us real-time information about cerebral perfusion during and after resuscitation. Wearables are entering the ED and perhospital arenas may soon place this data in our hands whether we want to learn transcranial ultrasound or not. We need to know what to do with this information when we have it.
5. Surviving Sepsis 2.0
Randomized controlled trials are already showing us that targeting easy-to-evaluate neurovascular goals in sepsis care may lead to patients surviving sepsis, but with fewer neurocognitive deficits than MAP goals alone.
6. Enhancing Clinical Decision-Making
From subarachnoid hemorrhage (SAH) to sickle cell disease (SCD), transcranial ultrasound empowers us with dynamic, spot neuromonitoring at the bedside. It complements neurological exams and CT findings, providing additional data for informed clinical decisions.
7. Portable, Cost-Effective, and Reproducible
Unlike CT or MRI, transcranial ultrasound requires no radiation, contrast, or expensive infrastructure. It can be performed at the bedside, in the ambulance, or even in austere environments, making it a powerful tool in resource-limited settings and disaster medicine.
It Is Time to Learn
We have long embraced innovation in point-of-care ultrasound. Many of the same objections some may have to evaluating the brain with ultrasound were once objections to non-cardiologists evaluating the heart. With its ability to rapidly assess brain perfusion, guide life-saving interventions, and the possibility of improving neurological outcomes, focused transcranial ultrasound at the point-of-care represents a new frontier. It is a tool at our disposal for answering focused, important questions, not a replacement for a neurologist or a CT scan. Learning this skill may not only elevate your clinical practice but also enhance patient survival and neurological recovery. Isn't it worth finding out more?